UW Bothell global public health class visits villages in Guatemala
Global public health students gained a new understanding of rural health care in the developing world

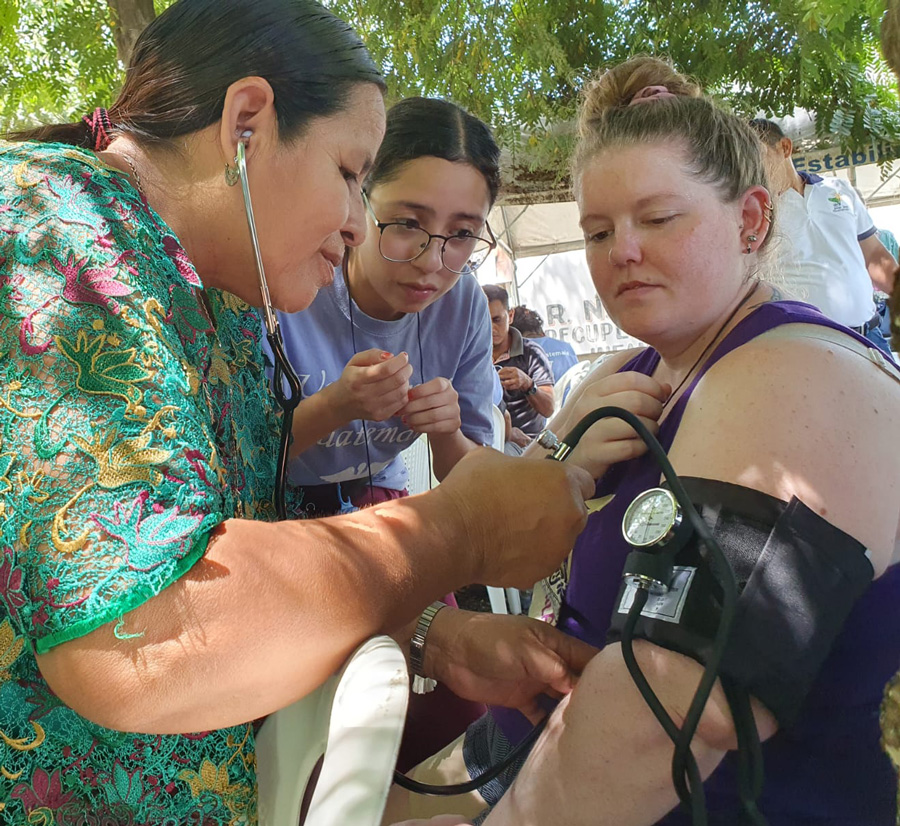
Student Leylani Blanco demonstrates how to take blood pressure measurements to health promoters and lay midwives. She was among 10 undergraduates and six master of nursing students who provided primary care and public health promotion in Guatemala this summer. Photo courtesy of UW Bothell.
Outfitted with boxes of medical supplies and purple T-shirts, students from UW Bothell traveled through Guatemala this summer, popping up clinics in rural Mayan villages and providing medical care and education to nearly 400 Indigenous people. Spending a few weeks in the villages, this contingent from a global public health class gained a precious understanding of rural health care in the developing world.
Students trekked to mountain and coastal villages, places where months could pass between visits from medical professionals. Arriving in trucks and SUVs to find residents lined up and waiting, they toted tubs of supplies into schoolrooms where they performed screenings and assessments and provided health education.
Guatemala has one of the world’s highest rates of child malnutrition, according to the United Nations Children’s Fund. Part of the UW group’s work centered on malnutrition assessments for babies and toddlers, providing nutritional supplements and health information to families.
“Clinic day is a bustling and dynamic environment, where patients receive personalized attention and care across a range of medical services,” says Leylani Blanco, a postpartum nurse who is completing her bachelor’s degree at UWB. While working with patients, Blanco gained insight into the health-care system of a different country and how the conditions where people are born, live, work and play affect their well-being.
Mabel Ezeonwu, ’03, ’08, a nurse practitioner and professor of nursing at UW Bothell, developed the class and led the trip. “This intensive hands-on service-learning course is designed to expose students to the policy contexts in which health care is delivered in remote resource-limited environments,” she says. With the community as the classroom, the students are challenged “to view global health-care issues holistically in order to understand how in-country health policies are influenced by local and global determinants.”
At each site, the students are assigned to a team that includes a doctor, nurse practitioner and other nurses. Each station is well-prepared to educate patients about their health conditions, perform medical assessments and administer treatments. The collaboration between different health-care professionals allows for a comprehensive approach to patient care.
- Photo courtesy of UW Bothell
- Photo courtesy of UW Bothell
The class works with Guatemala Village Health, a Seattle-based nonprofit cofounded by Dr. Jennifer Hoock, who completed her master’s in public health at the UW in 2008. The outreach organization has a mission to improve health in rural villages by providing access to medical care and health education, training health-care workers and implementing public health improvement projects. It brings teams of medical professionals from the U.S. to work with their local nursing team and train local health workers.
Community-based caregivers in southeastern and central Guatemala have long sought resources to train more health workers and midwives, but their local and regional governments haven’t come through. Through Guatemala Village Health, Hoock helped create a training program as well as the volunteer outreach health clinic that the UW students staffed.
“It is really a wonderful match,” says Ezeonwu of working with GVH. “The nonprofit gets engaged and experienced volunteers and the UW team gets community-centered experience and a chance to learn in another part of the world.”
“This class and trip have been an incredibly meaningful and beautiful experience for me,” says Blanco. “Collaborating with fellow nurses and individuals from various fields and backgrounds, each with unique values and interests has been eye-opening. Despite our differences, we came together as a team and forged genuine friendships.”